Uveitis describes a group of intra-ocular inflammatory conditions, where etiology is diverse and may be characterized by inflammation of the uveal tract or indirect inflammation of adjacent tissues1. In his paper, A Long-Term Game Plan for Non-Infectious Uveitis, Sam S. Dahr, MD, reports that the majority of uveitis cases seen in daily practice are non-infectious and idiopathic in origin. This report estimates that the disease affects approximately 300,000 American adults and 22,000 American children. Of great concern for the young, is the lack of proper treatment in the early stages of the disease, which can be attributed to a poor visual outcome 2.
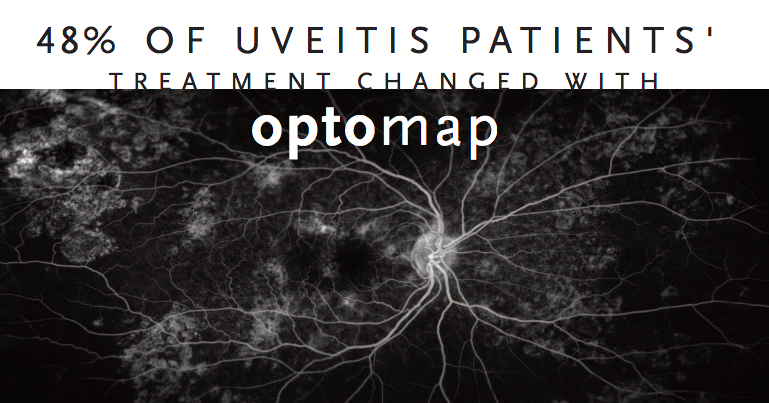
A study published in American Journal of Ophthalmology finds disease management
was altered in 48% of uveitis patients when optomap ultra-widefield imaging was used.
Proactive and effective management of non-infectious uveitis relies heavily upon developing a therapeutic strategy and a long-term plan, which may involve systemic therapy, patient counseling, close follow-up, dosing adjustments, combination therapy, and consultation with rheumatologists. In his report, however, Sam S. Dahr, MD, suggests that imaging metrics are “…more powerful than any blood test the rheumatologist can order to monitor response”; positioning ophthalmologists to “… bear the decision-making responsibility for these patients.” Many patients with non-infectious uveitis suffer “…inflammatory breakthroughs during systemic therapy, most of which tend to be fairly mild and treatable with topical, injected or oral steroids.” Having clinically-validated3 and efficient technology, such as optomap®, has a huge part to play in supporting the prompt follow-up and effective treatment in this group of patients.
There is growing evidence to support the value of optomap imaging for the detection of various pathological changes associated with non-infectious uveitis, which may alter patient management. Two independent studies utilizing ultra-widefield (UWF™) fluorescein angiography3 (optomap fa) and the autofluorescence (optomap af)4 modalities, respectively, determined that when compared to other imaging techniques and clinical examination, their findings influenced a change in some of their treatment decisions. Using optomap fa along with clinical examination influenced a revision in the treatment plans of almost half of the 43 patients (48 percent) in one study, compared to 7 of 43 patients (16 percent) based on examination and “limited fluorescein angiography.” Reznicek et al. concluded that the non-invasive optomap af modality detects more retinal or chorioretinal involvement and is, therefore, a useful diagnostic and follow-up tool in patients with uveitis. Other studies researching the utility of optomap technology in the management of patients with non-infectious uveitis, including the detection of vitreous haze5 and characterizing other associated retinal pathologies, have found it equally effective[6,7].
Given the prevalence of non-infectious uveitis in children disease detection and establishing a therapeutic strategy as early as possible is critical to reducing vision loss. Attempting to acquire retinal images from children with retinal disease, particularly when using the conventional or small-field imaging devices, has traditionally been difficult. A small study evaluated the value of UWF and the utilization of optomap fa in the pediatric population. Findings indicated that “…not only does including optomap fa reduce the need to bring patients to the operating room, but it also allows visualization of peripheral retina findings that are difficult or impossible with other imaging techniques”8.
optomap technology is an efficacious, clinically proven asset in the follow-up and treatment of all patients with non-infectious uveitis. The value of UWF imaging lies with its outstanding ability to image 82% or 200° of the retina in a single capture, which may be expanded, using it’s multi-capture, auto-montage functionality, which enables up to 220° of the retina to be imaged9. It’s non-contact, fast image capture, offering multiple modalities further support its value as a clinically relevant for the early detection of non-infectious uveitis, assisting in effective treatment management for patients of all ages.
Click here to discover the benefits of optomap (UWF) retinal imaging for your practice or clinic.
References:
- Rajen Gupta, Philip I. Murray (2006). Chronic Non-Infectious Uveitis in the Elderly Epidemiology, Pathophysiology and Management. Drugs & Aging July 2006, Volume 23, Issue 7, pp 535–558.
- Sam S. Dahr, MD (June 2017). A Long-Term Game Plan for Noninfectious Uveitis: Treatment requires patience and a nuanced approach. https://www.retina-specialist.com/article/a-longterm-game-plan-for-noninfectious-uveitis
- Campbell JP, Leder HA, Sepah YJ et al (2012). Wide-field retinal imaging in the management of noninfectious posterior uveitis. Am J Ophthalmol 154:908–911.
- Reznicek L, Seidensticker F, Stumpf C, Kampik A, Thurau S, Kernt M, Neubauer A. Systematic analysis of wide-field fundus autofluorescence (FAF) imaging in posterior uveitis. Curr Eye Res. 2014 Feb;39(2):164-71. doi: 10.3109/02713683.2013.834938. Epub 2013 Oct 21.
- Drew Dickson, Aniruddha Agarwal, Mohammad Ali Sadiq, Muhammad Hassan, Robin High, Quan Dong Nguyen and Yasir J. Sepah. Assessment of vitreous haze using ultra-widefield retinal imaging. Journal of Ophthalmic Inflammation and Infection 20166:35. https://doi.org/10.1186/s12348-016-0105-0
- Mesquida M, Llorenç V, Fontenla JR, Navarro MJ, Adán A. Use of ultra-wide-field retinal imaging in the management of active Behçet retinal vasculitis. 2014 Oct;34(10):2121-7. doi: 10.1097/IAE.0000000000000197.
- Paula E. Pecen MD, Kathleen F. Petro MD, Kimberly Baynes BSN, Justis P. Ehlers MD, Careen Y. Lowder MD, Sunil K.Srivastava MD. Peripheral Findings and Retinal Vascular Leakage on Ultra-Widefield Fluorescein Angiography in Patients with Uveitis Ophthalmology Retina, Volume 1, Issue 5, September–October 2017, pp 428-434. https://doi.org/10.1016/j.oret.2017.01.016
- Kai B. Kang, BA; Matthew M. Wessel, MD; Jianping Tong, MD, PhD; Donald J. D’Amico, MD; R. V. Paul Chan, MD Ultra-Widefield Imaging for the Management of Pediatric Retinal Diseases, Journal of Pediatric Ophthalmology and Strabismus. September/October 2013 – Volume 50 · Issue 5: 282-288. DOI: 10.3928/01913913-20130528-04
- https://www.optos.com/en/products/the-benefits-of-optomap/