One of the unique features of multiple imaging modalities, including color, fluorescein angiography (FA), fundus autofluorescence (FAF), red reflectance (RR), and indocyanine green angiography (ICG). Facilitating comprehensive examination of the retinal periphery, application of multiple UWF imaging modes can identify pathology that might otherwise be missed with a single imaging modality and/or conventional narrow-field fundus photography.
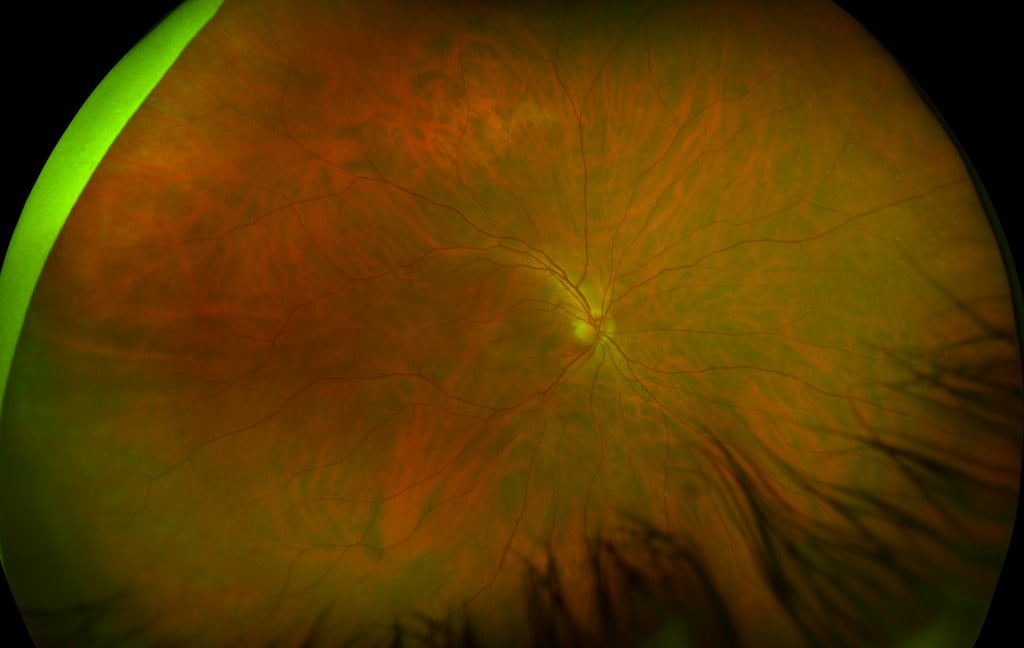
UWF color image of Central Serous Chorioretinopathy – California
A recent study, Ultra-Widefield Imaging with Autofluorescence and Indocyanine Green Angiography in Central Serous Chorioretinopathy1, demonstrates this capability using UWF FAF and UWF ICG in a central serious chorioretinopathy (CSC) retrospective observational case series.
CSC leakage from the choriocapillaris through the retinal pigment epithelium (RPE) causes macular detachment, which in turn can cause visual impairment or, in recurrent or chronic cases, blindness. Fundus autofluorescence (which can characterize the health of the RPE) and ICG chorioangiograpy (which can characterize choroid circulatory function) are both used in CSC diagnosis and treatment, but in the past have been limited to conventional, narrow-field views.
Study Subjects and Methods
The study examined 65 eyes (35 patients), all with CSC. Thirty-three patients had chronic CSC, which was defined as persistent/recurrent retinal detachment for more than 120 days and related RPE alteration.
All patients received comprehensive examinations including color fundus photography, UWF FAF, and spectral domain optical coherence tomography (SD-OCT). A smaller group (24 eyes) underwent UWF ICG chorioangiography.
Group Results
In 57% of eyes, UWF FAF detected peripheral disease that would otherwise not have been uncovered in a clinical exam or conventional, narrow-field FAF.
Additional findings included:
— In 5 eyes (6%), there was no evidence of active disease, but there were dark areas of hypo-autofluorescence that when compared with SC-OCT imaging showed photoreceptor loss, retinal thinning and RPE atrophy.
— In 16 eyes (24%), there was active disease. These were bright areas of hyper-autofluorescence, indicating increased metabolic activity in the RPE, and were correlated with SD-OCT imaging that confirmed the presence of sub-retinal fluid (SRF).
— In 44 eyes (70%), areas of hyper-autofluorescence were imaged but showed no related evidence of SRF in SD-OCT imaging.
— The UWF FAF images also showed gravitational fluid tracts in 32 (49%) of eyes.
Early phase UWF ICG showed that in 20 of 24 eyes (83.3%), outflow congestion of draining vortex veins was indicated by the observation of dilated choroidal vessels extending back to one or multiple vortex vein ampullas.
Individual Cases
The study also presented two cases in which UWF FAF and ICG were used to uncover the spread of CSC into the peripheral retina.
— In the first, a macular examination of a 43-year-old male with one-month history of central blurring of vision found no evidence of current SRF. An UWF FAF examination found two peripheral areas of hyper-autofluorescence, and follow-up SC-OCT imaging confirmed a diagnosis of CSC with findings of SRF and choroidal thickening.
— In the second, a 63-year-old woman with chronic CSC presented with persistent subfoveal SRF in one eye. Ultra-widefield revealed an area of hyper-autofluorescence at the macula and two more superior and inferior to the optic disk. SC-OCT imaging found SRF and choroidal thickening in all three areas. Ultra-widefield ICG imaging showed two areas of choroidal hyperpermeability, and reduced verteporfin photodynamic therapy was applied to these areas with good overall results and complete resolution of the macular SRF.
Implications for Practitioners and Researchers
For practitioners, the study’s authors emphasize that CSC, while classified as a macular disease, frequently involves the retinal periphery. Multi-modal UWF imaging with FAF and ICG can characterize the progression of CSC into the retinal periphery and even help identify areas in the periphery for treatment.
For researchers, the authors suggest that multi-modal UWF imaging may enable more in-depth studies of CSC, including (1) work to fully characterize and understand the progression and presence of peripheral hyper-autofluorescence even after resolution of SRF, and (2) UWF ICG studies to understand the possible relationship between the indications of outflow congestion of draining vortex veins and the severity of CSC.

Sources:
- Pang CE, Shah VP, Sarraf D, Freund KB, Ultra-Widefield Imaging with Autofluorescence and Indocyanine Green Angiography in Central Serous Chorioretinopathy, American Journal of Ophthalmology (2014), doi: 10.1016/j.ajo.2014.04.021.
- Definitions – hyper and hypo FAF: https://www.healio.com/optometry/technology/news/print/primary-care-optometry-news/%7B745b0a92-d46a-4804-a4f2-3a064115495b%7D/autofluorescence-imaging-allows-for-earlier-diagnosis-of-retinal-dystrophies