With glaucoma affecting as many as 4 million people in the U.S. alone and thousands upon thousands more around the world, it’s important for practitioners to be diligent in making sure patients understand their risk factors, as well as providing proper screenings to detect, diagnose, and monitor the condition.
In New York, Sanjeev Nath, M.D., had a 37-year-old female patient come in for an exam. She had a 20-year history of an “untreatable” retinal degeneration. At that time, she used high plus reading glasses and, with difficulty, was able to read magazine print from 4-inches. The patient felt her vision was worsening and also was experiencing difficulty seeing at night.
The patient’s vision was 10/400 in each eye unaided, and Goldmann IOP’s were 23 OD and 24 OS. An exam with a fundus with a slit lamp provided the explanation for her visual difficulties, and additional testing performed revealed Pachymetry to be 498u OD and 505u OS. Threshold fields showed the patient’s central Scotomas at about 12×15 degrees in size with erratic fixation. Her flash ERGs were normal.
However, the additional testing also revealed pisciform flecks and the appearance of the patient’s macula as presenting Stargardt’s disease. But because the patient’s flash ERGs were normal, Dr. Nath’s team knew another diagnosis would be necessary to explain the patient’s issues with her peripheral vision and her difficulties seeing at night. Doctors observed her discs and found asymmetric cupping, which indicated glaucoma.
While there’s no known treatment for Stargardt’s disease, glaucoma is treatable. However, in the case of this patient, all conditions had to be taken into consideration in order to develop the most appropriate course of action. This patient has been monitored carefully and the course of action that she chose was to have laser trabeculectomies in each eye supplemented with medications for the issue. Since the initial diagnosis, Dr. Nath has not seen evidence that either condition has worsened. Dr. Nath also takes optomap® images two times per year to continue monitoring the patient’s eyes, specifically keeping watch for changes in the patient’s mid- and far-peripheral retina.
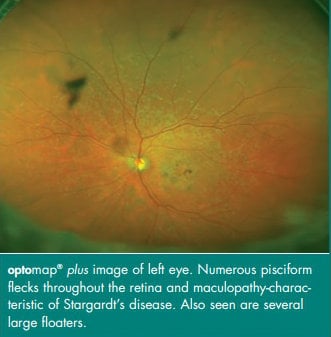
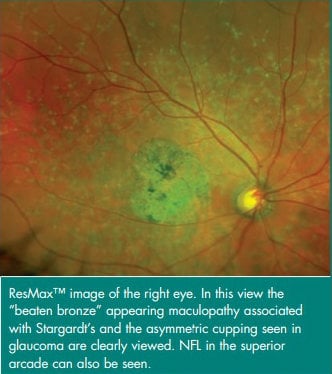
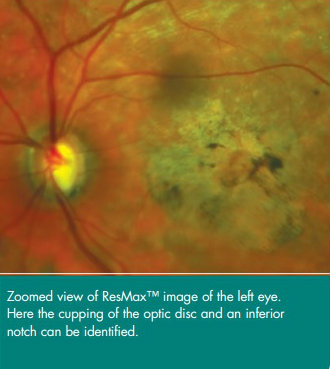
Practitioners interested in learning how our optomap ultra-widefield imaging can help diagnose and monitor retinal disease progression can contact us to speak with a representative for more details.